Capitol Correspondence - 10.29.18
Kaiser Family Foundation Issues 18th Annual Medicaid State Survey
Share this pageOn Thursday, October 25, 2018, ANCOR staff attended the Kaiser Family Foundation’s (KFF) event for the official release of its 18th Annual Medicaid State Survey (summary here, full report here). ANCOR encourages members to look at this report to advance your state and federal advocacy and stay up to date on the Medicaid landscape that informs policy-makers’ decisions on key topics such as Medicaid rates and eligibility.
Key highlights for policies relevant to the I/DD community:
- Medicaid policy-making in 2019 will be influenced by the results of state and federal elections, due to potential federal interest in capping Medicaid as well as ballot initiatives to expand the ACA. (Summary brief).
- 32 states increased provider rates for HCBS supports and services while 2 states decreased HCBS provider rates. This reflects a general trend of there being more states planning on rate increases in 2019 than states planning rate restrictions. (Pages 53, 56 of full report).
- CA, MD and RI added I/DD-specific HCBS benefits. (Page 46 of full report).
- LTSS trends:
- 48 states are seeking to expand the amount of people supported through home and community-based services (HCBS), including rebalancing tools, and most states seek to enhance benefits rather than reduce them. Specifically, expansion of HCBS includes: “use of HCBS waivers and/or State Plan Amendments (SPAs) (including 1915(c), Section 1115, 1915(i), and 1915(k)); use of rebalancing incentives in managed care contracts; use of Programs of All-Inclusive Care for the Elderly (PACE); and efforts to downsize state institutions. A large majority of states in FY 2018 (40 states) and in FY 2019 (42 states) reported adopting new HCBS waivers/SPAs and/or serving more individuals through existing HCBS waivers/SPAs.” (Pages 43-46 of full report).
- Recruiting and retaining a direct care workforce continues to be a large LTSS challenge for states. 24 states are planning wage increases for direct care workers in 2019, and 10 states are reporting new or expanded workforce development strategies. (Page 45 of full report).
- About half of states in the Money Follows the Person (MFP) program will discontinue services or administrative activities due to the grant expiring… But 30 states identified specific housing-related services that they plan to continue after MFP funding expires. (Page 47 of full report).
- 11 states are seeking to implement Section 1115 waivers with changes in eligibility requirements (including work requirements) and elimination or limitation of retroactive eligibility. Additionally, CO, IN, MO, NM and VT made changes specific to the “aged and disabled” category, including increasing asset limits. (Pages 7-8 of full report, and charts on pages 12-16).
- Managed care (MCO and MLTSS) trends:
- The Administration is expected to release revised federal managed care regulations by the end of 2018. (Page 19 of full report).
- Use of managed care for 75 percent or more of a state’s Medicaid population grew from 29 states to 33 states from 2017 to 2018. (Page 18 of full report).
- However, people with I/DD remain the least likely group to be enrolled in managed care on a mandatory basis – although Arkansas will include I/DD in its inaugural MCO program. (Page 21 of full report).
- 24 states offer managed long-term care supports and services (MLTSS), with almost every MLTSS state including both institutional and HCBS in the same contractual arrangement. This includes 7 states in which MLTSS was “always mandatory” for people with I/DD. (Page 48-49 of full report).
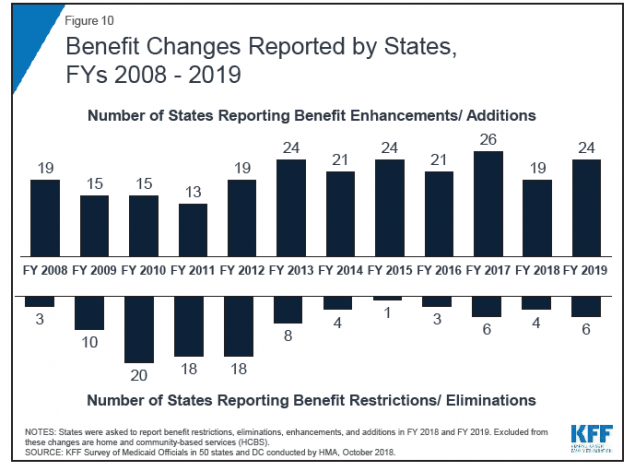
Image credit: Figure 10 of KFF full report.
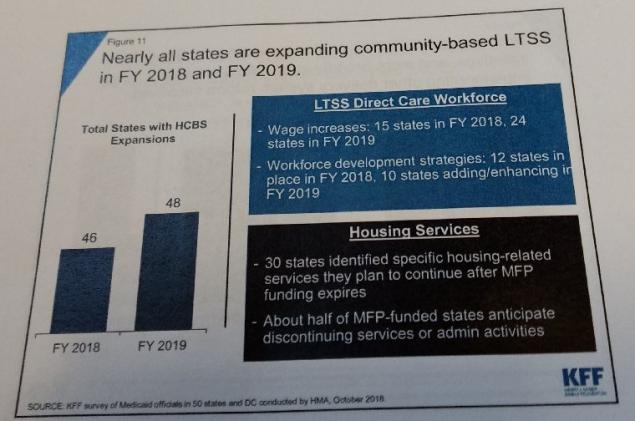
Image credit: Figure 11 in KFF presentation slides / issue brief.
